Key Takeways:
- Perimenopause disrupts sleep through hormonal changes that affect melatonin production, temperature regulation, and cortisol rhythm, making sleep lighter, more fragmented, and less restorative.
- Common patterns include trouble falling asleep, 3am wake-ups, early morning waking, and reduced deep REM sleep.
- Lifestyle adjustments help but have limits when hormones are the primary driver.
- Specialist support from a menopause-informed coach can identify what’s driving the disruption and address it properly.
When was the last time you had a really good night’s sleep? If you are in your late 30s to 50s and notice sudden changes in your sleep, such as struggling to fall asleep, 3am wake-ups, or simply waking unrefreshed even after a full night, it may be more than just bad sleep habits or stress.
Such changes in sleep are often linked to perimenopause, the phase leading up to menopause which affects 80-90% of women.
During this period of menopausal transition, fluctuating hormonal levels can affect how the body regulates sleep, temperature, and stress responses, often leading to hot flushes, night sweats and mood changes.
Why Am I Having Sleep Problems During Perimenopause?
Perimenopause is a phase marked by a gradual decline in ovarian function, leading to fluctuations in key hormones such as oestrogen, progesterone, and testosterone. These hormonal shifts play a significant role in sleep regulation, which is why sleep disturbances –including insomnia– become increasingly common during this stage.
The prevalence of sleep disorders ranges from 16% to 47% during the perimenopausal phase and increases to 35% to 60% in menopause. These changes are most strongly linked to oestrogen and progesterone fluctuations.
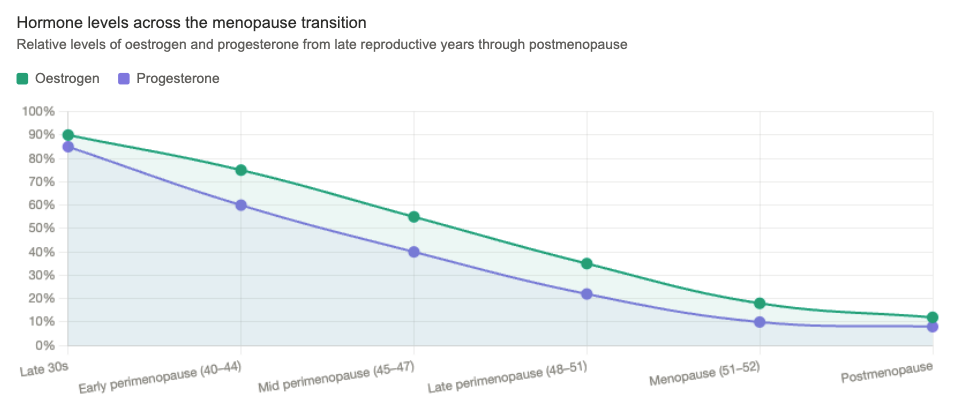
How Does Perimenopause Affect Sleep?
During perimenopause, the natural decline and fluctuation of oestrogen and progesterone can disrupt sleep in several ways:
- Difficulty falling asleep: Lower oestrogen can interfere with melatonin production, the hormone that signals your body it’s time to sleep. Progesterone normally has a mild calming effect, helping you relax and stay asleep. When both hormones fluctuate, falling asleep can become harder, and sleep may feel lighter.
- Frequent waking during the night: Hormonal changes make your nervous system more reactive, causing you to wake up more often.
- Early morning waking: Some women find themselves waking unusually early, around 4–5am, even if they are still tired.
- Disrupted sleep architecture: Perimenopause reduces the time spent in deep and REM sleep, the stages responsible for physical restoration and mental recovery. Even after a full night’s sleep, you may wake feeling unrefreshed.
When these issues become chronic, the effect on quality of life can be significant, impairing one’s wellbeing and physical functioning.
Why Am I Waking Up at 3am During Perimenopause?
Waking up at 3am is a common experience often linked to cortisol and blood sugar fluctuations at night.
Cortisol is your body’s primary waking hormone. It follows a natural daily rhythm, rising in the early morning to prepare your body to wake. During perimenopause, this rise can become exaggerated and shift earlier, making you alert at 3 or 4am when you should still be in deep sleep.
Having lower oestrogen makes the system that controls cortisol more sensitive, so it fires up in response to smaller changes than it normally would.
Blood sugar plays a contributing factor as well. When glucose drops overnight, your body releases adrenaline and cortisol to stabilise it, which can wake you suddenly.
Together, they make 3am waking a very common, if deeply inconvenient, feature of perimenopause.
Do Hot Flashes and Night Sweats Affect Sleep Quality?
Yes, and they can disturb sleep even on nights when you don’t feel very hot.
Hot flashes are sudden waves of heat caused by oestrogen fluctuations that confuse your brain’s internal thermostat. This thermostat becomes less precise during perimenopause, which means even small, imperceptible rises in core body temperature can pull you out of deep sleep, as your brain treats any temperature change as a signal to rouse you.
How To Sleep Better During Perimenopause
Improving sleep during perimenopause requires targeted adjustments.
- Keep a consistent wake-up time. Your circadian rhythm is anchored by your wake time, instead of bedtime. Getting up at the same time daily helps stabilise your sleep cycle.
- Support overnight blood sugar. Eat balanced evening meals with protein and slow-release carbohydrates to reduce the likelihood of a blood sugar dip that can trigger wake-ups.
- Cut caffeine earlier than you think. Caffeine sensitivity increases during perimenopause, so aim to stop by noon. Alcohol can also disrupt deep sleep and worsen night sweats.
- Cool your sleep environment. A cooler bedroom temperature is especially helpful when your internal thermostat fluctuates. Consider light, breathable bedding and moisture-wicking sleepwear.
- Exercise, but at the right time. Regular movement improves sleep quality over time but intense exercise late at night can make winding down harder.
- Calm your nervous system. A consistent 30-minute pre-bed routine, such as stretching, or a warm shower, signals to your body that sleep is approaching. This is particularly important when progesterone is low and your natural calming mechanism is weakened.
Why Doesn’t Sleep Hygiene Always Work for Perimenopause Insomnia?
Sleep hygiene helps, but when hormones are the primary driver, there’s a ceiling to how far lifestyle changes alone can take you.
If self-help has plateaued after four weeks, it’s worth seeking specialist support. Early intervention can prevent sleep problems from compounding and becoming more difficult to reverse. It is also valuable to rule out contributing factors such as thyroid imbalance, depression, or sleep apnea, which can co-occur in midlife women.
Prologue Wellness offers perimenopause treatments in Singapore where specialised menopause coaches take a personalised approach of assessing your sleep alongside your hormonal picture, lifestyle, and overall health to identify what’s actually driving the disruption. Where hormones are a significant factor, medical support is available as well, including hormonal blood testing and HRT consultations if appropriate.
Perimenopause sleep disruption is common, but it doesn’t have to be your new normal. With the right combination of lifestyle adjustments, hormonal awareness, and structured support, meaningful improvement is achievable – and with Prologue Wellness, you don’t have to figure it out alone.
References:
- Troìa L, Garassino M, Volpicelli AI, Fornara A, Libretti A, Surico D, Remorgida V. Sleep Disturbance and Perimenopause: A Narrative Review. J Clin Med. 2025 Feb 23;14(5):1479. doi: 10.3390/jcm14051479. PMID: 40094961; PMCID: PMC11901009.
- Polo-Kantola P. Sleep problems in midlife and beyond. Maturitas. 2011 Mar;68(3):224-32. doi: 10.1016/j.maturitas.2010.12.009. Epub 2011 Feb 3. PMID: 21295422.
